When the coronavirus pandemic first struck, The Life You Can Save established a special COVID-19 fund designed to help our recommended charities respond rapidly and effectively to the many different challenges posed by the COVID-19 pandemic. Gifts to the COVID-19 Fund were divided among ten of our recommended charities that developed special projects to address the COVID-19 pandemic: Development Media International, D-Rev, Evidence Action, Fistula Foundation, GiveDirectly, Living Goods, Malaria Consortium, Oxfam, Population Services International, and Project Healthy Children.
The support for this emergency COVID-19 fund has been strong. To date, our COVID-19 fund has generated $283,183 with over $240,000 of gifts coming in the first 3 months. These resources helped these recommended charities sustain vital operations and meet new, unforeseen needs in the communities they serve.
While our COVID-19 fund has been a great success and has helped our charities meet the urgency of the moment, The Life You Can Save has now closed this fund. The impact of COVID-19 on people living in extreme poverty is ongoing and will be felt for a long time. By now, however, we feel our recommended organizations have adjusted their operations to respond to our new reality. We therefore decided to close this special emergency fund and now recommend unrestricted funds to our recommended charities.
We wanted to highlight some of the wonderful work that your support has helped our recommended charities achieve. We recently asked our recommended charities that implemented special COVID-19 interventions to share some of the specific problems they faced due to COVID-19, the specific programs they put in place to overcome those challenges, and the ways COVID-19 has impacted their plans for the future. Below are their stories, which demonstrate the dedication, creativity and impact that our supporters have made possible.
DMI
We reached out to Cathryn Wood at DMI to learn more about how your support has helped them respond to the crisis:
DMI runs radio, TV and mobile campaigns to change behaviours and save lives. DMI was approached in early April by several governments with requests for assistance with tackling direct and indirect effects of COVID-19 on health outcomes. With the help of generous support from donors such as GiveWell, the Mulago Foundation and the Skoll Foundation, as well as from individual donors through The Life You Can Save, DMI was able to respond quickly to this emergency and undertake robust, impactful COVID-19 campaigns in all nine of its countries of operation.
Thus far, DMI has produced 56 radio spots in 37 languages, an animation on social distancing, a live action film on mask wearing, and a live action film on social distancing. DMI estimates that this COVID-19 content has reached 40-45 million people in sub-Saharan Africa. Evidence from previous trials suggests that these campaigns will result in a 10% increase in respiratory and hand hygiene behaviours in the region and that this increase — as well as reductions in social contacts also promoted by the same campaigns — will help significantly mitigate the spread and impact of the pandemic in sub-Saharan Africa.
What’s Next:
As COVID-19 continues to grip Sub-Saharan Africa, the demand for health services has dropped, and this decrease in demand is projected to have a significant negative impact on health outcomes in the region. WHO has stressed that campaigns that aim to increase the demand for essential health services where available are a priority at this time. And where these services are unavailable, mass media can be used to promote healthy behaviours in the home.
DMI’s aim is to run campaigns to combat the indirect health effects of COVID-19. The indirect effects will vary from country to country; for example, in Côte d’Ivoire the government has asked DMI to help tackle falling vaccination rates while in Uganda DMI has been approached regarding a spike in teenage pregnancies. The precise themes of DMI’s campaigns will be dictated by the need and health service capacity in each country, as determined by governments and DMI’s formative research.
Equalize Health (D-Rev)
Equalize Health (D-Rev) has published two updates on their COVID response. Here The Life You Can Save Communications Manager, Adam Sneed, summarizes some of the key points:
In response to the COVID-19 pandemic, Equalize Health (D-Rev) has resolved to strengthen its focus on maternal health solutions and uphold its commitment to “creating technology for everyone, so that no matter where an expectant mother lives, she has access to world-class medical treatment.” Read more about the problem of preventable maternal deaths, how COVID-19 threatens to exacerbate that problem, and the steps Equalize Health is taking to mitigate the virus’ impact.
In November 2020, Gauri Singh, a Commercial Manager for Equalize Health, published a vivid account of how her own personal struggle with COVID-19 intersected with and informed her professional experience working with frontline healthcare workers to understand and meet their needs. Singh writes, “My experience has strengthened my commitment to the mission of Equalize Health. Together, we can create a world where everyone, no matter where you live, has access to world-class medical treatment.” Read more…
Evidence Action
Evidence Action recently published updates on their COVID response. Here The Life You Can Save Communications Manager, Adam Sneed, summarizes some of the key points:
Evidence Action’s COVID-19 response has been quite different from their standard approach to scaling high-impact and cost-effective programs. In line with their commitment to ‘thinking big and acting urgently’, Evidence Action quickly pivoted to address critical gaps. When COVID-19 lockdowns began taking effect in March 2020, Evidence Action’s Dispensers for Safe Water team rapidly compressed three months’ worth of program deliveries into just two weeks to ensure the communities they serve would have uninterrupted access to safe water if logistical networks shut down. At the same time, Evidence Action purchased soap and disinfectant from suppliers in major cities, and rented a fleet of trucks to transport them to their field offices. From there, their circuit riders – using motorbikes to reach even the most remote villages – passed the supplies on to their promoters.
Evidence Action also conducted training for promoters on COVID-19 symptoms and prevention strategies (such as good handwashing practices and social distancing), and worked with them to identify frequently touched places in their area. Promoters then took responsibility for disinfecting these surfaces 3–4 times per day, and for distributing soap and key messages to households in their community. Between March and July 2020, Evidence Action delivered over 924,000 liters of chlorine for treating drinking water; over 3 million kilograms of soap for handwashing; over 99,000 liters of disinfectant; and nearly 44,000 informational stickers to promote good hygiene practices. They are extremely grateful to The END Fund, The Waterloo Foundation, The Clorox Company, The Life You Can Save, Latter-day Saint Charities, and other generous donors for their support of this work.
The urgency of the COVID-19 pandemic has meant that Evidence Action had to adapt their monitoring and evaluation approach accordingly. Evidence Action’s monitoring protocols usually entail conducting household visits to collect information and test water samples for the presence of residual chlorine (households that test positive are assumed to have treated their water with chlorine from the dispenser). During the pandemic, they have had to limit in-person data collection to reduce the transmission risk for their staff and communities.
In addition, a lack of widespread COVID-19 testing in their catchment areas means that Evidence Action had to rely on proxy measurements, such as self-reported incidences of respiratory symptoms. Though self-reported data may carry a ‘social desirability bias’ (respondents over-reporting socially desirable behavior), they determined that this is the safest and most appropriate data collection method in the context of COVID-19. Evidence Action’s Monitoring, Learning, and Evaluation team is conducting a correlational and trend analysis of self-reported behaviors, and validating these by comparing them to self-reported data on the incidence of respiratory and other COVID-19 symptoms. As part of this, their team have conducted phone interviews with a sample of 451 promoters and 1,757 households in Kenya; 290 promoters and 1,104 households in Uganda; and 281 promoters and 1,106 households in Malawi.
Preliminary data indicates high levels of knowledge of handwashing with soap for 20 seconds as a prevention strategy, and most households reported our promoters as key sources of COVID-19 messaging. However, Evidence Action has observed a gap between high rates of handwashing knowledge and lower rates of effective handwashing practice. They are continuing to investigate why this might be, including through additional data collection and analysis, and hope to have more to share soon. Nonetheless, the rates of effective handwashing are considerably higher than those shown in recent Demographic and Health Surveys from the same areas; there may be an opportunity here to explore possible drivers of this behavior change, and whether these gains could be sustained beyond the COVID-19 crisis.
Fistula Foundation
We reached out to Katie Weller at Fistula Foundation to learn more about how your support has helped them respond to the crisis:
When Covid-19 began to spread around the world earlier this year, Fistula Foundation feared that the pandemic and its economic fallout could decimate the already fragile healthcare systems of low-income countries across Asia and Africa. Although we are usually laser-focused on fistula treatment alone, we knew that something had to be done. In May, we amended our legal charter to allow us to raise emergency funds for Covid-19. We immediately sent 100% of gifts to this newly established fund to our partners on the ground. Generous donors enabled these hospitals to safely provide essential health services and lead community prevention efforts during the pandemic.
We originally set out to raise $450,000, but the response from donors far exceeded our expectations. Since beginning this effort in May 2020, we’ve raised more than $690,000. This was an outpouring of 1,300 gifts from donors across the globe who wanted to help our partner hospitals stand strong during the pandemic.
Thanks to our donors’ generosity, our heroic doctors have been able to continue their essential work. We immediately distributed the funds to 24 partners in twelve countries across Asia and Africa. These funds have been used to purchase essential personal protective equipment (PPE) and infection control training and supplies and to maintain staff salaries, prevent layoffs and keep hospitals open. Thanks to this support, most of our partners have returned to full functionality and resumed fistula treatment after initial shutdowns.
One such partner is Dr. Sunday Lengmang, the lead fistula surgeon at Evangel Vesico-Vaginal Fistula Center (EVVF), our trusted partner hospital in Nigeria. Like so many of our partners, Dr. Lengmang’s team has been hit hard by the Covid-19 pandemic. Amidst economic hardship, EVVF was forced to close entirely— until they received a grant from our Covid-19 Emergency Response Fund. Thanks to Fistula Foundation’s generous supporters, Dr. Lengmang and his team are back to helping women in need!
“We are overwhelmed by your extraordinary grace in providing additional support to our work in Nigeria… Thanks to Fistula Foundation donations, our patients and health care workers are well protected.” -Dr. Sunday Lengmang, lead surgeon at EVVF Hospital

What’s Next:
Despite this good news, the crisis is far from over. Restrictions on travel and gatherings because of the pandemic have made it even harder for women to give birth in a hospital or access emergency obstetric care. As a result, we worry that more women than ever are at high risk of developing obstetric fistula. We remain committed to the women who are counting on us for treatment—and to enable that important work, will continue to support our partners hardest hit by Covid-19. Together, we can help these partners emerge strong and remain the force for good they’ve always been treating obstetric fistula.
Give Directly
We reached out to Anna Cerf at Give Directly to learn more about how your support has helped them respond to the crisis:
The economic impact of COVID-19 across Africa has been severe, with those living in extreme poverty put into even more vulnerable positions. In emergencies like COVID-19, cash reaches recipients quickly, safely, and efficiently. Needs vary drastically, and cash lets families address their most pressing need — be it rent, food, healthcare, childcare or something else that donors or the broader aid sector might not be able to anticipate.
GiveDirectly quickly adapted our model – which, in the past, had four in-person touchpoints – to launch 100% contactless COVID-19 responses that delivered emergency cash to families in need. By quickly incorporating new components such as SMS enrollment, machine-learning targeting and remote recipient verification into our model, we were able to scale programs to reach more than 350K recipients and deliver cash safely and efficiently to recipients across varied contexts, from refugees in Rwanda to those affected by Hurricane Dorian in the Bahamas. Overall, we were able to raise more than $215M for recipients and to deliver $0.88 of every dollar directly to recipients. Our first results from a basic income study in Kenya showed that recipients had improved well-being despite the pandemic. And results from a benchmarking study in Rwanda suggest that direct-cash payments outperformed a job training program, at the same cost, across all metrics except production of business knowledge.
What’s next:
In 2021, we’ll continue to deliver cash to those affected by COVID-19, while leveraging models built this year to scale up. Our standard lump-sum programs will continue to reach recipients in more remote locations, reaching those who other NGOs might not be able to reach, with an updated light-touch model. Our next set of results for the basic income study will be released, and RCTs will continue across countries. We will continue cash-to-refugee projects and be prepared for humanitarian disasters. Through it all, we’ll advocate for cash as a powerful, evidence-backed, anti-poverty tool that empowers recipients to define their own solutions.
“I’m overjoyed because we were hopeless and held back by poverty, but now things are going to change for the better. We thought you wouldn’t come back because of the COVID-19 pandemic… I have no doubt we will make great use of the fund we will be given.” – Uyisabye, recipient in Rwanda (pictured below)

“I sleep on dried banana leaves and a grass mat which often gives me back pain. After receiving the GD grant, I bought these mattresses for me and my daughter and grandkids. I’m happy and grateful that GD helped my family sleep better.” – Marie Grace, recipient in Rwanda (pictured below (R) with her daughter(L))

Living Goods
We reached out to Ashley Brekke at Living Goods to learn more about how your support has helped them respond to the crisis:
The COVID-19 pandemic has exacerbated and overwhelmed existing health care systems. Current estimates reveal over 1.4 million confirmed cases and more than 32,000 deaths in Africa. For African families who live on wages of less than $5 a day, the economic and health impacts of this pandemic are severe. Disruptions in essential health service delivery within already weak healthcare systems lead to additional preventable deaths; for example, Uganda witnessed a hike in maternal deaths due to pregnant women’s inability to reach health facilities during lockdown.
Living Goods adapted to the challenges of the COVID-19 pandemic quickly to continue ensuring essential health services in communities. With the goal of ensuring continuous care to that communities and individuals who are at the highest risk of experiencing the negative impacts of the COVID-19 pandemic, Living Goods determined three key pillars to guide our response efforts: (1) protect frontline health workers so they can educate their communities and interrupt COVID-19 transmission; (2) maintain and expand essential health services so that no additional preventable deaths occur due to COVID-19 response; and (3) support governments with national response efforts to create more resilient health systems far beyond this pandemic. We enacted no- and low-touch protocols to enable over 11,000 community health workers (CHWs) to continue safely providing essential health services. We focused on continuing care, such as immunization, family planning and disease prevention, in order to avoid excessive deaths. We assessed nearly 892,000 sick children under five years and supported almost 50,000 new mothers before, during, and after pregnancy. We also screened 144,285 households for COVID-19 (with only 213 suspected cases), and referred 24,727 suspected COVID-19 cases in Uganda (with only 21 positive cases). Overall, we estimate that we improved health outcomes for over 8 million people.
What’s Next:
COVID-19 has highlighted for governments the crucial role played by primary health systems and has made clear that the effectiveness of these systems begins at the community level. As we look ahead, our key focus areas will be engaging effectively with governments, running impactful experiments, continuing to build our internal technology capacity, and acting as thought leaders for the community health field. We will measure success in terms of how we contribute to: (1) increased, rigorous evidence for the impact of technical assistance on community health program performance; (2) governments incorporating best practices into their community health programs and financing mechanisms; (3) organizations overseeing community health programs thinking about per-CHW impact; and (4) a consensus on the great benefits of using mobile technology and data-driven decision-making to support community health programs.
Human Interest Story
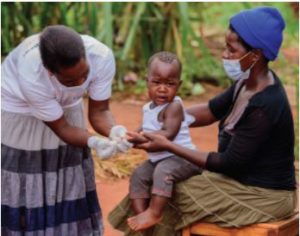
Hasifa lives in a village near the shores of Lake Victoria in Buikwe, one of the border districts that have been most affected by COVID-19 in Uganda. The nearest health center is quite far from her home. There are clinics within a walkable distance, but their services are costly and therefore exclusionary. When her children fall sick, Hasifa calls upon Shamidan, a Living Goods-supported community health worker (CHW) who lives a few houses away. “I usually come to this CHW because she treats my children, whether I have money at hand or not. Before she started giving us free medicines, her prices were fair compared to the clinics,” Hasifa says.
Before the pandemic, Shamidan was already a trusted CHW in the community. But her role has become even more crucial now, as she continues to diligently support the health needs of children and women and educate her community about COVID-19. “She listens to our needs. There would be a big gap without these CHWs in our communities. This CHW used to check on me almost daily when I was pregnant and ensured that I accessed the necessary antenatal care. Without her, the situation would have been dire because I had a complication and she accompanied me to the hospital, on time. We need her,” Hasifa affirms.
Shamidan is one of two CHWs in her village and serves more than 200 households. She has been instrumental in maintaining the delivery of essential reproductive, maternal, newborn and child health (RMNCH) services in a community with many mobile households that are engaged in fishing activities. Since April 2020, she – like other CHWs supported by Living Goods – has received free essential medicines to treat sick children for common illnesses, such as malaria, diarrhea and pneumonia. She also receives personal protective equipment (PPE), including gloves, masks and sanitizers, to ensure her safety.

“What I like most about my job is that the clients I treat believe in me. That motivates me. I also get incentives every month, without fail,” Shamidan says, adding that she is proud of her work and looks forward to the day COVID-19 will end so she can fully resume door-to-door service. Her biggest concern now is that when Living Goods stops distributing free medicines, her clients might not be able to afford buying them as they were able to before the pandemic.
Malaria Consortium
Malaria Consortium recently published updates on their COVID response. Here The Life You Can Save Communications Manager, Adam Sneed, summarizes some of the key points from those updates:
When the WHO declared in early March of this year that COVID-19 had reached the stage of a pandemic, governments and communities mobilized to respond. Their actions have been key in isolating cases, slowing disease transmission and easing the burden on overextended health systems.
But these measures could also cause serious disruptions to health services for other diseases, such as malaria, HIV and tuberculosis, particularly in low- and middle-income settings. Response measures such as restrictions to movement or home confinement, physical distancing and diversion of resources to cope with the increased demand on health systems could severely impact health seeking behaviors, the delivery of existing interventions (such as net distribution to prevent malaria infection) and diagnosis and treatment of other communicable diseases.
Global efforts to halt the spread of the pandemic and alleviate pressures on healthcare systems have made clear that our emergency response efforts must promote and facilitate the continued delivery of existing essential healthcare services, not compromise it. Containment efforts can be sustained, and even enhanced, by harmonizing them with current interventions.
Malaria Consortium’s 2020 seasonal malaria chemoprevention (SMC) campaign in Nigeria demonstrates how it is possible to adapt, and act, to support vulnerable communities during the COVID-19 pandemic. Working alongside the Government of Nigeria and global and national stakeholders, Malaria Consortium has worked to develop detailed guidance on safe implementation of SMC in the context of COVID-19. This has included limiting in-person contact and social distancing, improved health education — a core element of the campaign — and providing face masks and hand sanitizer to SMC implementers. Malaria Consortium estimates that these adaptations will help to prevent up to 962,000 malaria cases and 9,600 malaria deaths, strengthen national and state capacity to respond to the pandemic and create more resilient health systems overall. They will also ensure the continued provision of preventive and diagnostic malaria services to those most vulnerable to malaria infection — children under five.
Read Malaria Consortium’s advocacy brief from October 2020 to find out more about these adaptations and our recommendations for national and state governments and implementing partners.
Oxfam
We reached out to Claire Beynon at Oxfam to learn more about how your support has helped them respond to the crisis:
The COVID-19 pandemic is wreaking untold havoc on many communities around the world. In many places where Oxfam works, public health and hygiene are already compromised by limited access to clean water and sanitation. The people in these communities are especially vulnerable to the spread of coronavirus and other infectious diseases.
But when disaster strikes, Oxfam acts. And thanks to a massive outpouring of support from our donors, we’ve joined forces with local organisations across the globe — from Bolivia to Mozambique to Bangladesh — to stem the spread of the virus in places already besieged by poverty.
Globally, the Oxfam confederation has reached more than 11 million people in 62 countries with COVID-adapted programming this year. Together, we’ve deployed many practical and creative solutions to empower affected communities to defeat this new invisible enemy. We’ve collaborated with national authorities, local authorities and village committees to distribute vital COVID-19 safety messages on social distancing and hand-washing practices. And we’ve developed public health messages that address the unique needs of marginalised communities, including people with disabilities and people with non-binary gender identities.
Here’s a global “snapshot” of Oxfam’s coronavirus response:
- In Bangladesh, we are reaching some of the most vulnerable communities with food, public health awareness-raising, hygiene kits and protective equipment.
- In Papua New Guinea, we are increasing our hygiene awareness work and scaling up delivery of clean water, soap and sanitation supplies. We are also sharing information with communities about the gender impacts of the pandemic.
- In Timor-Leste, a specially approved cargo plane has delivered hundreds of handwashing kits and public health information packs.
- In Iraq, our humanitarian staff and local partners are training health workers, distributing personal protective equipment and hygiene kits, and delivering thousands of public information brochures.
- In Zaatari refugee camp in Jordan, we are working to reach 78,000 people with water, hygiene, and sanitation resources.
- In Vanuatu, we are working with our local partner organisations to identify locally-appropriate ways to share COVID-19 preparedness messages.
- In Pakistan, with local partners we are providing support by distributing hygiene kits and running a communications outreach campaign.
- In Indonesia, we’re distributing hygiene kits, developing public handwashing facilities, and providing clean water by restoring or protecting existing water sources.
Population Services International
We reached out to Beau Westbrook at PSI to learn more about how your support has helped them respond to the crisis:
PSI works to strengthen and build health systems around the world to help individuals live healthier lives and plan the families they desire. Though PSI has made great strides in the last 50 years, the coronavirus pandemic posed significant threats in countries with already-fragile health systems by overwhelming existing infrastructure and frontline health workers. The COVID-19 pandemic put an urgent halt to many of PSI’s essential healthcare delivery methods, such as in-person services and product distribution. From the beginning, we recognized that a lack of information and outright misinformation during a pandemic could be extremely dangerous and result in people being less protected from the spread and that individuals at all levels of the healthcare spectrum – from consumers to community health workers to Ministries of Health – would need timely, fact-based information about how to prevent, detect and manage the virus to keep their families and communities safe and healthy.
Building off our experience with other outbreaks such as Ebola, cholera, and Zika, PSI teams recognized that a crucial first step was setting up a cross-functional team based at PSI’s global headquarters tasked with PSI’s central COVID-19 response. Made up of a cross-section of experts from PSI’s clinical, research, operations, safety and security, digital and communications departments, the team was able to respond to quickly changing environments and updated findings from internal research and external best practices and information. PSI’s internal response team outlined a global response strategy that has been adapted to work within different cultural and epidemiological contexts across PSI’s network of 50 countries. Our approach was threefold: to continue to deliver, as effectively as possible, essential support and services through innovative methods such as digital healthcare and self-care; leverage experience and expertise in behavior change communications expertise to design effective communication and clinical training packages for COVID-19 prevention and control; and implement long-term solutions that strengthen health systems to better manage the next disease outbreak.
We focused in on our key strengths to address the gaps within the healthcare system across our network: designing culturally-driven communications campaigns to spread factual, timely information, to increase prevention and connect people to COVID-19 testing sites, as needed; using digital technology to help individuals access information, self-diagnose and get help as needed; delivering digital training to healthcare providers on COVID-19 testing and treatment in real time; and working with Ministries of Health to strengthen data surveillance, emergency operations and management information systems. We developed COVID-19 guidance across multiple health areas and implemented 318 unique program adaptations globally to integrate COVID-19 prevention measures, support frontline service providers and ensure continuity of essential health services during the COVID-19 pandemic. We also launched social behavior change campaigns that reached 30 million+ people in over a dozen countries and provided them trusted information on COVID-19 prevention. Modifications to our distribution strategies such as introducing a mobile payment system for volunteers and a proprietary app for tracking stock enabled us to distribute 98% of the expected 7.8 million insecticide-treated nets in Mali.
What’s Next
While COVID-19 safety guidelines and operating procedures are still a shared reality across PSI’s network, we plan on focusing attention and efforts on vaccine hesitancy in 2021. Through surveys and consumer insight gathering we’ve done over the past six months, PSI understands that hesitancy and misinformation associated with the COVID-19 vaccine could prevent a safe and effective rollout. The panel surveys that we have conducted have helped us identify clear opportunities for intervention through effective campaigns that will inform and influence behavior change among individuals and frontline health workers and address barriers such as political interference, mistrust of large industries, rumors, and misinformation.
Human Interest
Hadiya* lives in a remote village in Pakistan, miles from the nearest health center. Due to the pandemic, her family’s financial situation has become more precarious by the day. Her husband is a daily wage earner and had not been able to work since the lockdown started in Pakistan. Hadiya worries about her family’s future and knew one thing to be certain: she could not afford to have more children.
Hadiya has never used contraception and wasn’t sure where to access it, until she received a visit from a PSI-trained health worker. The health worker, Lubna, introduced her to a PSI Pakistan initiative that is providing safe access to modern contraceptive methods even during the pandemic. Hadiya was able to procure a long-term contraceptive method that will help protect her from unplanned pregnancies for the foreseeable future. “It is good to have someone who cares about you and your health,” Hadiya said.
Project Healthy Children
We reached out to Felix Brooks-Church at Sanku-Project Healthy Children to learn more about how your support has helped them respond to the crisis:
At Sanku-PHC, we aim to end malnutrition using technology and a business model that lets the small mills that feed the most malnourished people conveniently and affordably fortify staple grains. Our mission is to guarantee that every meal consumed by every mother and child contains vital nutrients, forever.
COVID-19 and its ripple effects have put millions of children at risk of malnutrition; making the urgency for scaling our cost-effective, sustainable solution greater than ever. As a small social enterprise, the Covid-19 crisis forced us to ask 3 important questions:
- Can Sanku-PHC survive?
- Can we maintain impact?
- Can we assist with the Covid-19 response?
Thanks to the loyal support of our donors and the robustness of our model, we can answer a resounding YES to all three questions.
- Sanku-PHC not only survived; we grew. The team returned safely to the field in July and have been joined by some exciting new recruits, including an exceptional COO who will help Sanku-PHC build the team and systems we need to achieve our goal of reaching 25 million people with fortified flour by 2025.
- Over the course of the year, we continued to support our existing partner mills and worked with 80+ additional mills; each new mill having the potential to increase our reach by 6,700 people.
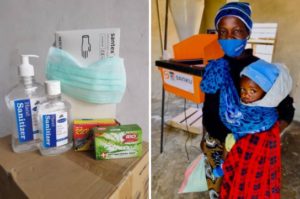
- We helped protect our partner millers, their staff and families by supplying hundreds of health kits packed with protective gloves, masks, antibacterial soap and hand sanitizer, including over 10,000 masks made from empty flour bags that would otherwise have gone to waste.
- We partnered with USAID to run two “Fortification Road Shows” to address supply chain disruptions caused by Covid-19; working with schools and village millers to fortify 34,000kg of maize and raising awareness about Covid-19 and the importance of good nutrition through an SMS campaign, households visits and posters – reaching over 7500 families.
Most importantly, Sanku-PHC continued to ensure that thousands of families were able to access flour fortified with lifesaving vitamins and minerals, including immunity boosting zinc. Our sincere thanks to everyone who supported us and made that possible.